How To Read An EKG (electrocardiograph)
 Today I found out how to read an EKG.
Today I found out how to read an EKG.
While some people might say that kind of skill should require 13 years of preparatory school, four years of college, four years of medical school and a specialty in cardiac electrophysiology, I say…Pshaw! It’s not rocket science! If it were, there would be more combustion and potential for speedy projectiles gone awry (You know, I bet rocket scientist Christmas parties are really fun…and imagine the Fourth of July company picnics!)
This is just cardiology, simple biological pipes and wires. EKGs are simpler still, being a moving real time map of the “wires” part and how they conduct electricity. Reading EKGs only seems hard because most cardiologists use long (expensive) words.
As a warm up for the rest of this article, you might want to take a gander at Today I Found Out‘s article: “How The Heart Works”. Or, to make a long story short, most healthy hearts pump blood through the body when stimulated by an electrical signal that travels along predetermined pathways. This causes the cardiac cells to contract in just the right order, resulting in a magical four chambered pumping action.
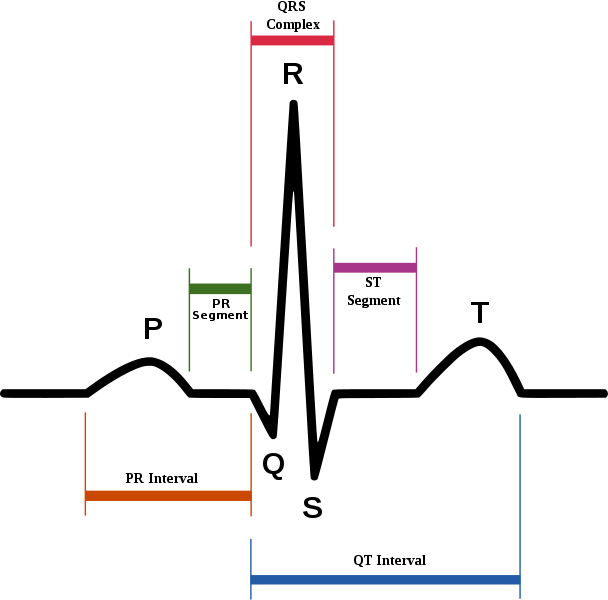
An EKG is a graph (thusly named an electrocardiograph) tracing the strength and direction of this electrical signal. Leads equipped with conductive goo are placed on different parts of the body allowing a view of the heart from different angles. If the electrical activity of the heart at any given moment is traveling toward the lead being viewed, the line on the graph goes up (positive deflection). If the electrical activity is traveling away from the lead, the line goes down (negative deflection). This graph is being traced by a stylus on a moving piece of graph paper. In a normal healthy heart, an EKG representing one complete heartbeat looks about like this :
That first petite little hump, affectionately called the P wave, represents the electrical signal that starts in a group of cells called the Sinoatrial Node. This signal then travels through the atria (the smaller and upper two chambers of the heart) causing them to contract and push blood in to the larger and more powerful ventricles below.
The “PR Interval” segment represents a delay in the signal at another grouping of cells called the AtrioVentricular Node. This delay allows time for the atria to completely deliver their bounty into the Ventricles. With perfect timing this signal continues through the Bundle of His. The signal splits and speeds along down the left and right bundle branches, making its way to the Purkinje fibers and turning north again. This stimulates those Ventricular beefcakes to contract and deliver their payload to the lungs and body (if hearts had biceps, the left ventricle would be the proverbial “gun show”….it’s such a glory hog!).
The journey causing this second contraction through the ventricles is represented by the QRS portion of the EKG. The larger T wave which then finishes off our heartbeat is the repolarization of the ventricles. I know what you’re thinking, either “what in the what now goes where?” or hopefully, “what wave represents the repolarization of the atria”? Well, the repolarization of the atria is buried in the larger signal of the QRS and therefore not visible on the graph.
This pattern is called normal sinus rhythm. It is the basic EKG of any normal healthy heart. Naturally, there are variations of normal within the healthy population. For example, my boyfriend is very fit and has a *huge* R wave (hands off his big left ventricle ladies, it’s all mine! And don’t get me started on his early repolarization…and no…being early in this case is definitely not a bad thing).
However, anything outside of the normal range is analyzed along with the patient’s symptoms to create a working diagnosis. There are several types of common abnormalities. A PR interval that is too long is called a first degree block. A QRS that takes longer than .12 seconds is likely to be caused by a delay in one or both bundle branches, called a bundle branch block. A complete lack of P waves, and in their place a squiggly line, combined with an irregular heartbeat is likely to be atrial fibrillation. What really gets a Paramedic or ER doctor excited is when they see an elevation of the ST segment in a few consecutive leads. This is referred to as an ST elevation myocardial infarction (heart attack) and generally results in a speedy trip to the catheterization lab (if you’re interested in more of what is going on during a heart attack, see: How a Heart Attack Works). Truly, the list of irregular EKGs is endless.
To bastardize the words of Leo Tolstoy, who seemed to know a thing or two about the heart, “Happy [hearts] are all alike; every unhappy [heart] is unhappy in its own way”. If only Anna Karenina’s troubles could have been solved by a trip to the cardiologist!
Bonus Facts:
- Each small box on the modern EKG strip represents 0.04 seconds on the horizontal axis.
- EKG paper is calibrated to move at 25mm per second past the stylus.
- The EKG was invented by the Dutch Dr. Willhelm Einthoven in 1903, for which he received the Nobel Prize in 1924. More impressively, he also had a triangle named after him.
- It is very rare, but possible for an EKG to show a flat line, called asystole, when in fact the heart is still beating and producing a pulse. It is because of this that it’s common practice to confirm death in a patient by looking for asystole in more than one lead.
- Conversely it is also possible, and more common, to have an EKG show heart activity, and even normal sinus rhythm, after a person has died and their heart is no longer pumping blood. This is called a PEA, pulseless electrical activity, and shows what is left of the heart’s intact electrical system after the muscle itself has failed.
- The coffee stimulated brains of two nerdy paramedics with way too much time on their hands.
- The Hearts Electrical System
- Sinus Rythm
- Image Source
| Share the Knowledge! |
|





I’m delighted you have cracked one of the greatest myths of all time, namely that medicine is not rocket science at all. All you need to know is how the body is supposed to work and deduce what has gone wrong when it doesn’t. The most popular ECG (sorry I am from the UK) guide is entitled “The ECG Made Simple” and is almost compulsory reading for all medics. If medics caqn understand it then anyhbody can!
Nice write up. I’d say you have some flawed thinking to assume you have learned everything there is about the EKG in a day. 13 years (although in the U.S. its 4 years of medical school, 3 years Internal Medicine Residency, 3 years cardiology fellowship for a total of 10 years….14 if you add in the 4 years of college before med school I guess) is training the physician to understand everything there is about the body so they can deduce what is wrong and in the case of the cardiologist it is a lot more than understanding why simple science behind a P wave, QRS complex, and T wave. The genius method of the EKG is quite simple; however, it takes much more practice to be able to determine the many different cardiac pathologies by the reading of an EKG. Yes. It is easy to understand the basics in a day. Correlating what you see from the 12 leads to a full understanding of cardiac physiology, in coordination with the rest of human physiology of concern is what takes many years. Don’t fool yourself, doctors aren’t trying to fool you into thinking they could have been trained in way less time. They shouldn’t be. And anyone who tells you differently is probably just a Nurse Practitioner (lol. jusssst kidding).
@Will: It should be noted that the author of this article is a paramedic and has been for many years. 🙂
Seeing how it’s over in 10 seconds makes me think it’s worthless. Well not just that. In 2010 I had my aortic valve replaced. (EKG Normal) This past Wednesday I had a heart catheter. They found blockages and scar tissue. (EKG Normal) It took 3 years dealing with the doctors to find out what “Chest Pain” meant. It’s not always a sharp searing pain. Sometimes it’s a heaviness in he chest. A feeling like you’re walking through molasses, not air. All the while…. EKG NORMAL
@Chuck: That’s why many tests should be run, not just the EKG. However, EKG does give an amazing amount of information about a lot of problems as described in the article.
@ Chuck, Like Daven said, its just one test that should be combined with other tests, its not the end all be all. EKG is just to measure the electrical firing of the nodes in the heart. If you’re having a valve problem or blockage, your nodes could be firing normally and your EKG appear normal, but your blood pressure would most likely be higher than normal among other test results.
You shouldn’t give people this false advice that its easy to read an ECG. What you’re talking about is a NORMAL ecg ryhtm. Even a slight shift in any of the complexes, the time, the distance, can mean so many things. What about the Leads that are used for the ecg, Lead 2, Lead 3, Ave, etc. Please be clear, you have shown how to read a NORMAL ecg on ONE lead. If you want to learn how to read ecgs, try YouTube. They have some videos there that might be of interest.
@Anonymous: Given the author is a paramedic who teaches classes on how to read EKG’s, I don’t think what he’s saying is false advice. And you’ll also notice many abnormalities are covered.
When did being a paramedic make you an ECG specialist?
This is in the same realm as comparing Grey’s Anatomy to Gray’s Anatomy.
@pQRSt: Paramedics have to be extreme experts on EKG’s because they have to be able to look at one and try to rapidly deduce from what they’re seeing what’s going on in a patient, often in emergency situations under high pressure. When doctors do them, they often have a lot more time to analyze what they’re seeing. From my personal experience with this (having a pretty mysterious heart condition that’s been looked over by paramedics and doctors alike many times over the years, including by the author of this article, Scott), I can say that the paramedics were able to deduce more from the EKGs, and much quicker, than the doctors. One of Scott’s co-workers even figured out I have a concave chest within seconds of seeing one of my EKGs Scott took, which was kind of interesting I thought. 🙂 It’s really amazing how much they can figure out just by looking at a little chart of electrical activity within the heart.
I had a car crash today. The ambulance face me narcaine but I don’t use herion or opiodes. I was at fault hit car head on. I remember everything up to the ambulance
Not to knock Doctors and their education, I am an EMT, and I would question how many Doctors could Actually pass an exam to become a Paramedic. I know mine couldn’t!!! I have seen a lot of RN’s fail a simpler EMT exam. It is kind of like a professional baseball player trying to hit a fast-pitch softball, they think it would be easy, but it is very hard to do.
I am an paramedic turned MD. Let’s be honest here, being an paramedic is not “that” hard, I did it for many years. It is high stress but the knowledge an paramedic holds pales in comparison to an MD. I am not surprised honestly, first of all paramedics are field trained operatives, unless you are an EM trained trained doctor, any other MD would likely fail a paramedic exam b/c they are not emergency specialties. Particularly for medical specialty, most of the doctor’s work is in his/her brain, it is cognitive, it is thinking about it in a million different angles. Doctors have an absurb amount of education and trust me when I say we know a lot more then you guys in most aspects.Even an EM doc failing a paramedic exam does not matter. They are EXAMS, paramedicsl cannot claim to do what EM docs do.
Grammar and attention to detail must not be taught in your med school.
What if the R wave gets super small a few times?
As a medical student I’ve spent the past few days studying ECG … (It’s rocket science). 🙁 😀
what happens if the P wave is negitive?
Then your heart is firing backwards, which would hurt a lot because your basically having a heart attack.
Does anyone know if you have had a avib await ion if that would effect a major surgery like colon resection. I’ve been cleared for a yearly check up so I haveeb symptom free…anybody ?
Can I just say I loved the way this was written, because it was a lot more light hearted and not so serious with a quirky comment here and there keep me interested I picked this up quite fast, cardiac rehab exam is going to be a breeze!. I researched bundle of HIS and everything made sense
Well written…if only all medical books could be written like this. Although, this only took a few to pick up…the heart is a complex organ…so with that said the EKG is only a small fraction of the study. But very well written…thanks for puttin it together 🙂
Well, he has got a good description about what normal looks like. If it ain’t normal, like he says something is wrong and more tests are in order. Yep, he’s right about the atrial fibrillation. graph freaking the ER staff out. I was there just a few days ago. They Like quick wheeled the “crash cart up to the door while they were working on me, my pulse went straight through 140 to 166 and the graph was little tiny triangle waves wandering all over the screen. They were having trouble with a quick connect for an I.V. line and were getting kinda shakey and had two people working on getting that quick connect forced together. Suddenly Snap and in came the Digoxin, Bam! Down went the heart rate and my chest loosened up. Then one more tiny dose and I was down to 130 and the staff was visibly more relaxed quit worrying about having to sweep up all those springs and ball bearings off the floor and trying to put the mess together. Medicine plus a Cardiovert (heart stoppage and restart) Straightened me out. Still on O2 but with no load I can do without.
Personally, I would more quickly put my life in the hands of most paramedics, Physician Assistants (or even a veterinarian) than most doctors (whether 12, 14 or 40 years of education/experience).
Even in Scott’s “very simplified” but enlightening explanation of the heart and its function, it is readily apparent that such a complex design of instrument and operation could never have just evolved. Such intelligent design could not have ‘just happened’ at once or over a series of efforts. And to think that the heart and its operation is only a singular part of an organism with a myriad of other such amazements which all work together leads one to think that there must have been an exceptionally intelligent Designer of this thing called the human body when the first one was created a living being. This sure makes it difficult if not impossible to deny something like an all-knowing God had a very significant role in this, doesn’t it?
Hi, I went to the doctor and he did a EKG and said my T was bad and walked over to a Cardiologist. Cardiologist said we needed to investigate. unfortunately stress test and echo is scheduled in two month and I am concern because I don’t understand what the t is telling the doctor, am I getting ready for a heart attack?
Thanks for helping to break it all down for me. I am not in the medical field, but have been dealing with an array of medical issues, the most recent of which was inappropriate sinus tachycardia with elevated BP. I was admitted to the ER with a sustained HR of 180 for over half an hour with my BP bouncing all over the place like a toddler who’s had too much chocolate. I’m still looking for answers, and am trying to collect as much data as possible while also gaining a passing understanding of the information I’m collecting. Thanks for the help!
My heart doctor said once that I have possibly a minor bundle branch block but I shouldn’t worry about it. I did research, but never got close to this level of clarity and information intensity you present here.
I learnt a lot in a few minutes. Thank you!
my thoughts exactly. well written!!